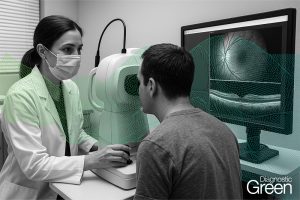
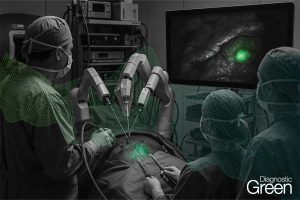
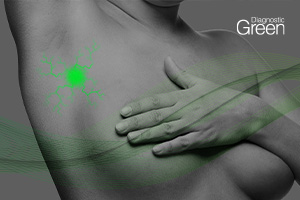
Background: Mastectomy skin flap necrosis is a major complication of skin- or nipple-sparing mastectomy. Indocyanine green angiography (ICGA) is a novel technology that can identify flaps at risk of necrosis, but there is paucity of cost-effectiveness data particularly in the Australian context. We evaluated its cost-effectiveness in breast reconstruction surgery.
Methods: Single-institution retrospective study of 295 implant-based breast reconstructions using ICGA compared with 228 reconstructions without ICGA from 2015 to 2020. Costs were calculated using Medicare item numbers and micro-costing analysis. Break-even point analysis determined the number needed to break-even. Cost-utility analysis compared probabilities of ischaemic complications and utility estimates derived from surveys of surgeons to fit into a decision model.
Results: There were 295 breast reconstructions using ICGA with a total cost of AU$164,657. The average cost of treating an ischaemic complication was AU$21,375. Use of ICGA reduced the ischaemic complication rate from 14.9% to 8.8%. Ischaemic complications were prevented in 18 breasts resulting in gross cost savings of AU$384,745 and net savings of AU$220,088. Three hundred eighteen cases using ICGA are needed to break-even. The decision model demonstrated a baseline cost difference of AU$1,179, a quality-adjusted life-years (QALY) difference of 1.77, and an incremental cost-utility ratio (ICUR) of AU$656 per QALY favouring ICGA.
Conclusions: Routine use of ICGA during implant-based breast reconstruction is a cost-effective intervention for the reduction of ischaemic complications in the Australian setting. ICGA use was associated with a gain of 1.77 additional years of perfect health at a cost of AU$656 more per year.