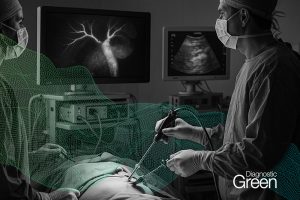
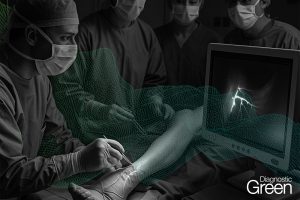
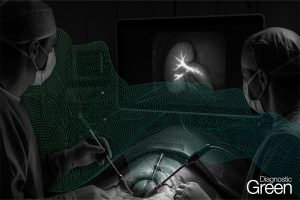
Laparoscopic cholecystectomy (LC) is one of the most frequently performed gastrointestinal surgeries worldwide. Bile duct injury (BDI) represents the most serious complication of LC, with an incidence of 0.3%-0.7%, resulting in significant perioperative morbidity and mortality, impaired quality of life, and high rates of subsequent medico-legal litigation. In most cases, the primary cause of BDI is the misinterpretation of biliary anatomy, leading to unexpected biliary lesions. Near-infrared fluorescent cholangiography is widely spreading in clinical practice to delineate biliary anatomy during LC in elective and emergency settings. The primary aim of this article was to perform an up-to-date overview of the evolution of this method 12 years after the first clinical application in 2009 and to highlight all advantages and current limitations according to the available scientific evidence.
The results of the current up-to-date overview confirmed the efficacy of ICG-fluorescence cholangiography in detecting biliary anatomy, its importance as a teaching tool for young surgeons, and the effects on the reduction of conversion rate and BDI, even if further considerable research remains necessary to optimize its use. This frontier method has enormous potential to become the gold standard during all cholecystectomies in elective and emergency settings due to its safety and limited costs. However, clear clinical guidelines are necessary for the surgical community.